Pulseless electrical activity3/22/2023  However, this did not improve the infant’s HR. After auscultation indicated cardiac arrest with PEA rhythm chest compressions, four doses of epinephrine and two boluses of 10 mL/kg of normal saline were administered. Initial mask ventilation, MR SOPA (M –mask adjustment, R –reposition airway, S –suction mouth and nose, O–open mouth, P–pressure increase, and A–airway alternative) and intubation were provided with no change in HR. This represented the presence of an HR on ECG of 80–90/min. The infant’s Apgar score remained at 1 at 1, 5 and 10 min after birth. However, since the 2015 guidelines changes, the authors of this case series have witnessed several newborn infants presenting with cardiac arrest with PEA rhythm.Īn extremely low birthweight infant was born via emergency caesarean section for antepartum haemorrhage. 12 Cardiac arrest with PEA rhythm has not previously been reported in newborn infants. 11–13 In adults, PEA occurs in approximately 35%–40% of in-hospital arrests and 22%–30% of out-of-hospital cardiac arrests and is associated with a 2%–5% survival to discharge rate. 11 Narrow QRS complex PEA might be due to cardiac tamponade, pulmonary embolism, tension pneumothorax or mechanical lung hyperinflation, 11–13 while wide QRS complex PEA is more likely due to electrolyte disturbances, tachydysrhythmias, cardiomyopathy or cardiac ischaemia. 11 Furthermore, PEA is categorised as narrow QRS complex (70% of cases) or wide QRS complex. Depending on the electrical origin, PEA can be classified as sinus, atrial, junctional or ventricular. The occurrence of cardiac electrical activity with no associated mechanical activity is called cardiac arrest with PEA rhythm. 8 Furthermore, we have reported two animal studies with cardiac arrest with PEA rhythm, where ECG displayed an HR ranging between 15/min and 80/min in 23/54 9 and 22/30 10 asphyxiated piglets. 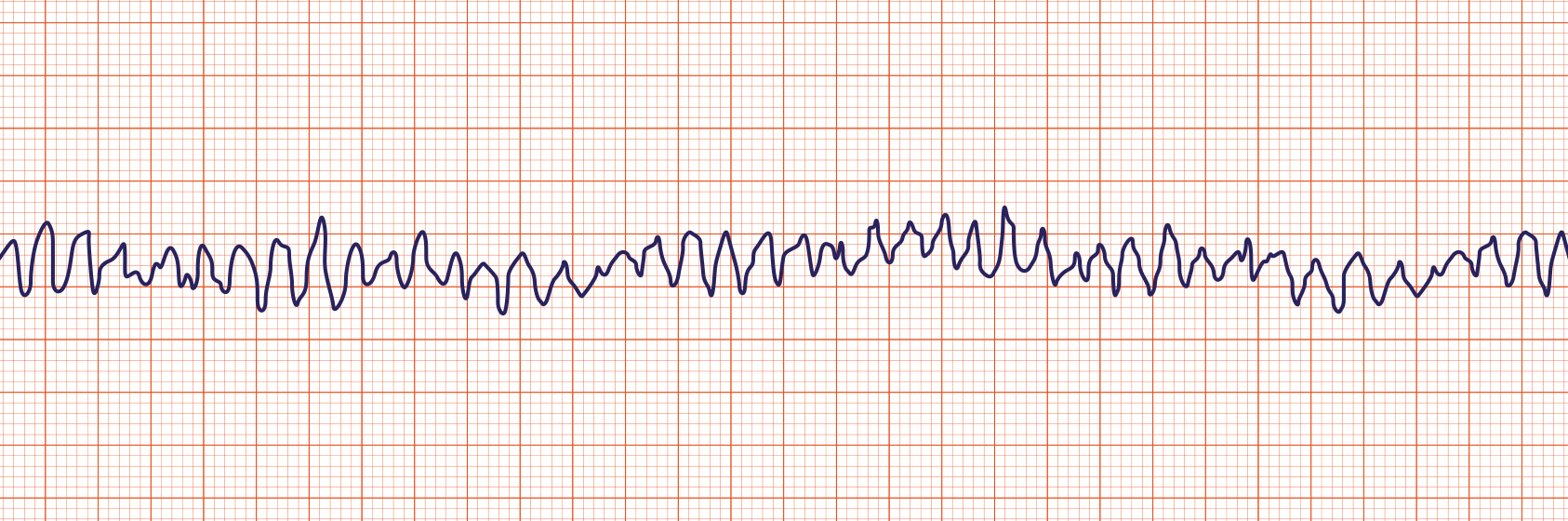
One followed placement of a central catheter resulting in cardiac tamponade 7 and the second occurred during neonatal resuscitation. 6 In addition, two case reports reported pulseless electrical activity (PEA) in newborn infants. 3–5Ī recent case report of a newborn infant with hydrops fetalis raised concerns about the reliability of ECG. 1 2 However, this weak recommendation was based on low-quality evidence, that is, observational data and small randomised trials. 1 In 2015, the neonatal resuscitation guidelines changed their recommendation to suggest using ECG to assess an infant’s HR immediately after birth. 1 Until recently, HR in newborn infants at birth was assessed using: (1) palpation of the umbilical cord, (2) auscultation of the precordium and/or (3) pulse oximetry. 1 Increase in the newborn’s HR remains the most reliable indicator of adequate ventilation. Heart rate (HR) is the most important clinical sign to evaluate compromised newborn infants and to guide resuscitation efforts in the delivery room. When ECG displays a heart rate but the infant is unresponsive, pulseless electrical activity should be suspected and chest compression should be started. Furthermore, in compromised newborns, heart rate should be assessed using a combination of methods/techniques to ensure accurate heart rate assessment. We propose an adapted neonatal resuscitation algorithm to include pulseless electrical activity. Healthcare providers should be aware that pulseless electrical activity can occur in newborn infants during cardiopulmonary resuscitation. We report four cases of pulseless electrical activity during neonatal cardiopulmonary resuscitation in levels II–III neonatal intensive care units in Canada (Edmonton and Winnipeg ). 
However, a recent case report raised concerns about this technique in the delivery room. 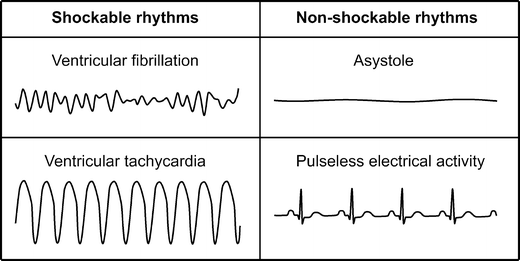 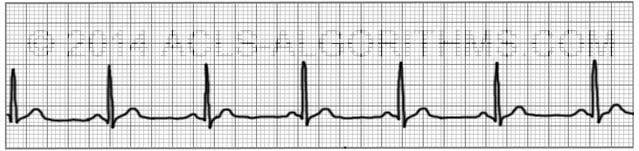
The 2015 neonatal resuscitation guidelines added ECG to assess an infant’s heart rate when determining the need for resuscitation at birth. 
0 Comments
Leave a Reply.AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
